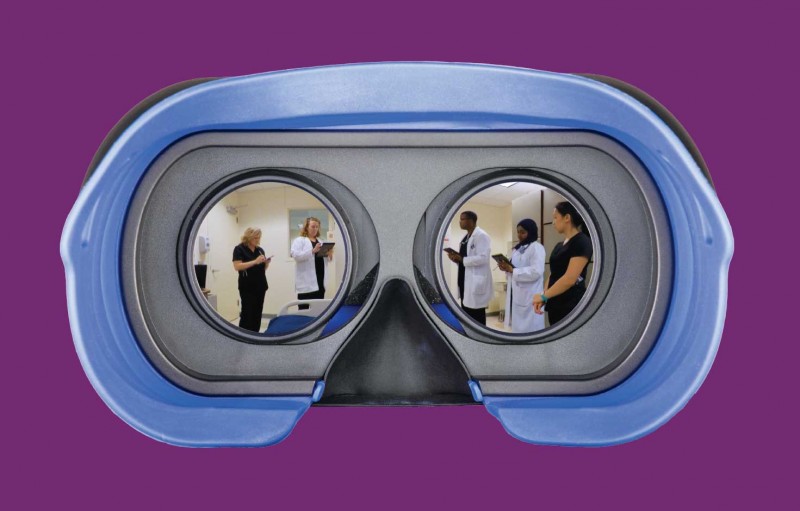
Virtual reality helps nursing students experience a patient’s perspective
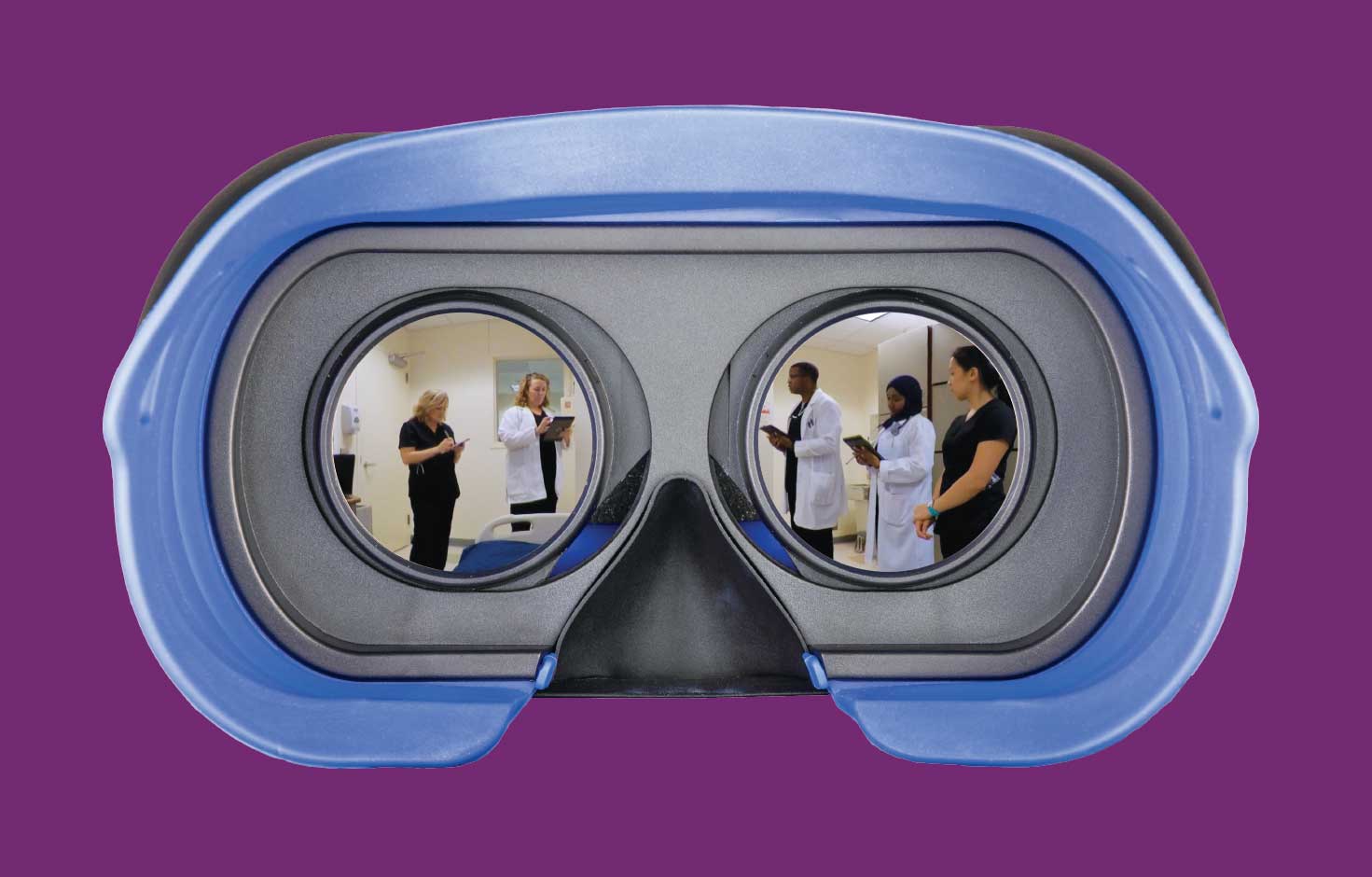
At the click of the door, a weary mother shrugs off a white blanket at her daughter’s side. A medical team files in, curt and professional.
White count not coming down. Some epithelial sloughing. A significant pulmonary injury. Her CRP is elevated. Consider ECMO. Let’s ready her for transport.
The mother tilts her head, trying to take in the words but unable to find the sense in them. Rapid-fire questions about her daughter’s vaping habit leave her stunned and confused. As she begins to weep, the team files out of the room. The mother turns to the last person remaining: the nurse sedating her daughter.
“What does all that mean? Just tell me what’s going to happen to her, please!”
“Mrs. Kelly, I have to go check on a patient, but I’ll be back as soon as I can,” the nurse responds, then she, too, walks out the door.
The scene is as heartbreaking to witness as it is common.
“Many of us have experience with loved ones interacting with the healthcare system and not receiving the kind of care we felt they needed in terms of empathy,” reflects Clinical Assistant Professor Lori Sprague, also assistant director of the Innovative Simulation and Practice Center at Binghamton University’s Decker College of Nursing and Health Sciences. “And we thought, ‘Maybe we can help people understand what it’s like to be that person going through the experience.’”
A virtual reality (VR) simulation helps undergraduate nursing students do just that, by allowing them to experience an emergency-care scenario from the perspective of an intubated patient. The scenario is intended to instill empathy that, contrary to popular belief, is a skill that can be acquired and strengthened.
An innovative solution
Decker has explored VR’s possibilities before, but earlier software was expensive and involved a full headset tethered to a computer. Limited to a single user at a time, it proved unfeasible for a classroom setting or home use. Enter the smartphone, the YouTube app and Google Cardboard.
“You really need to be able to reach the masses, so we came up with this idea of creating a virtual reality simulation that is easy and accessible,” says Patrick Leiby, Decker’s director of technology and innovation. “You can get a $3 cardboard headset, put your phone in it and have 100 students all sitting in a room at the same time, doing the same virtual reality simulation.”
Collaborative Research in Simulation and Practice (CRISP), a research group that includes both Sprague and Assistant Professor Rosemary Collier, won a SUNY Innovative Instruction Technology grant for the project. Collier and Sprague are also part of an interdisciplinary research group on tobacco use and drew on their knowledge to create the vaping scenario in partnership with nursing programs at SUNY Delhi, SUNY Broome and SUNY Brockport.
“It was right around this time that we were seeing some of these lung-injury cases, such as young people getting ‘popcorn lung’ and ending up in the ICU after using vaping products,” says Collier, also an emergency care nurse in the Binghamton area.
Unlike traditional video production, VR must be shot in a single take; to stay out of the scene, Leiby worked in a separate room, operating the camera from an iPad. The parts were played by faculty members, who practiced during several dress rehearsals before Leiby filmed the scenario with an Insta360 camera.
For their roles, the faculty members drew on aspects of their own experience. The day before the filming, Sprague’s daughter was admitted to the hospital for a medical emergency; captured in the video, her feelings as a distraught mother were fresh and raw. Collier, who played the lead physician, is deeply familiar with the communication blind spots that can sometimes occur in an emergency setting.
“If you’re ever in a critical care unit, physicians walk around with these teams of residents, respiratory therapists and a nurse, going from room to room,” Collier recounts. “They have a job to do, and the job isn’t always therapeutic communication with the patient and family.”
Empathy in the curriculum
So far, the VR simulation has been part of the Introduction to Professional Nursing course, where goggle-wearing students watch and then discuss the simulation together.
Empathy and emotional intelligence are part of the nursing curriculum, and they are developed in diverse ways. For example, nursing students learn how to physically transfer patients to a bed while practicing on each other, which not only imparts skill, but gives them insight into what a patient feels: in short, empathy.
“I’m comfortable in a healthcare setting; it’s my home base. But for every patient who comes through that door, it’s a terrible day, their worst day. It can be hard to remember to put yourself in their shoes and to remember that this isn’t their home base,” Collier says. “You really have to go out of your way to create some connection and comfort.”
When Jenny Nigro lifted the goggles to her eyes, she was already feeling stressed from competing deadlines and a big test later that afternoon. As she watched the scenario unfold, she was struck by the patient’s vulnerability.
“It was a meditation on empathy to see how the care team’s brusqueness and lack of warmth resulted in (the patient’s) experience of helplessness,” says Nigro, who graduated with her nursing degree in May 2022. “In the post-brief, I noted how timely it was that our empathy VR simulation was occurring on a day when we were feeling overworked and tired. It offered an opportunity to reflect on how we might manage these feelings that will likely come up in nursing practice, so that we do not disempower our clients.”
Plans are in the works to create additional VR scenarios, such as ones involving patients who don’t understand English or situations that might require conflict-resolution skills. Leiby has also used the 360 technology on other projects, such as a virtual tour of Decker’s new Motion Analysis Research Laboratory.
Virtual reality scenarios can play an important role for future nurses, allowing them access to experiences they may not encounter during their clinical time and sharing those experiences with classmates, Collier points out. At its heart, sharing is the foundation of empathy.
“Patients don’t always remember the clinical complexities occurring behind the scenes, but they will remember how their nurse or provider cared for and treated them,” Sprague says. “Sometimes it’s just a matter of pulling up a chair or changing your body language and respectfully giving a few moments of your time.”